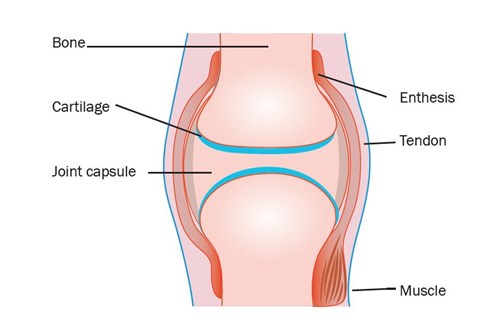
If you have Crohn’s or Colitis, your immune system can cause inflammation in the joints and the area around them. This relationship between your joints and your Crohn’s or Colitis is sometimes known as the gut-joint axis.
It is not fully understood why this happens. Research shows that it may be genetic, meaning it runs in families.
Spondyloarthritis is also more common in people who have a particular gene called HLA-B27. Your doctor may do a blood test to see if you have this gene.
Many people do not realise that there can be a link between joint and gut symptoms. Your GP or IBD team may not always specifically ask about joint problems. This can mean arthritis may not be diagnosed for some time and effective treatment can be delayed.
There are different treatment approaches depending on the type of arthritis you have and if you are having a flare-up of your gut problems. See treatments for more information.
Other causes of joint problems
Not all the joint problems you experience may be related to Crohn’s or Colitis. Side effects of some medicines used to treat Crohn’s or Colitis can affect the joints. Other causes include injury, infection or other types of arthritis, so careful investigation is important.
Medicine side effects
Infliximab
Common side effects can include joint pain, muscle pain and back pain.
Steroids
Stopping steroids too quickly can cause joint pain. Long term steroid use can also damage the joints (especially the hip joint) – see osteonecrosis.
Azathioprine
Joint pain can happen if your body is sensitive to azathioprine. It usually starts within three months of starting the medicine. Your doctor may recommend that you switch to mercaptopurine.
If you have started a new medicine and have joint pain, check the Patient Information Leaflet that comes with your medicine to see if this could be a side effect. Let your IBD team know.
Osteonecrosis
This is a rare but serious side effect that can produce joint pain. It happens when steroids cause problems with blood supply to a bone, usually in the hip or knee. You may need medicine or surgical treatment.
Injury
Joint pain can be due to injury such as a sprain or strain during exercise. Find out more on the NHS website.
Gout
This is caused when uric acid crystals are deposited in the joints. It causes sudden and painful attacks usually in the joints of the foot, knee, ankle, hand and wrist. It is very common in the big toe.
Find out more about gout on the NHS website.
Infection
Inflammation of a joint can be caused by bacterial infection. This is known as septic arthritis, and is rare but a medical emergency.
Germs can enter a wound and travel through the bloodstream to infect a joint or may infect a joint directly after an injury or during surgery.
Usually a single joint is affected. Symptoms include sudden redness and swelling around a joint and a high temperature.
You are more at risk if you are taking immunosuppressant medication to treat your Crohn’s or Colitis.
Find out more about septic arthritis on the NHS website.