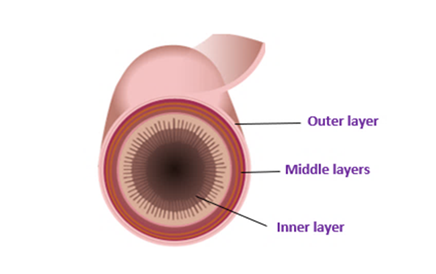
Advancement flap
The inside of the fistula is removed and the tract cleaned. The hole where the fistula joined the bowel is then covered with a flap. This flap is formed from the lining of the rectum, which is end of the bowel.
This operation is used for complex fistulas. This operation is also used when fistulotomy would carry a high risk of losing bowel control.
LIFT (Ligation of Intersphincteric Fistula Tract)
This operation aims to avoid cutting the sphincter muscle. The surgeon accesses the space between the internal and external anal sphincter muscles. This is done through a small cut at the entrance to the bottom. Once the surgeon has found the fistula tunnel it is cut in two. Both ends are then stitched closed to stop poo getting into the fistula.
VAAFT (Video-Assisted Anal Fistula Treatment)
Using a telescope camera, the surgeon can see the fistula track from the inside. After cleaning, the fistula track is closed using an electric current. Stitches and fibrin glue can also be used. This technique also helps surgeons find extra passages running off the main fistula. These extra passageways also need treatment for the fistula to heal.
Risks of anal fistula surgery
Like any surgical procedure, surgery for anal fistulas has some risks. The main risks are:
- Infection
- The fistula comes back (recurrence)
- Loss of bowel control (incontinence). This is a potential risk with most types of anal fistula treatment. Severe incontinence is rare. Your surgeon will make every effort to prevent this.
The level of risk will depend on where your fistula is and the type of operation you have. Talk to your surgeon about the possible risks of the operation and the benefits that it can offer you. You will have an appointment with a surgeon prior to any operation.
Other treatments
Other treatments include closing the fistula with a special medical glue or paste. A plug made from materials like Gore-Tex® can also be used to cover the hole. Sometimes medical laser probes are used to seal the tract shut.
Stem cells
Stem cells might be effective in treating complex perianal fistulas in mild Crohn's. Stem cells could be useful if medicines have not worked, or someone does not want to have surgery. But this treatment is not approved for use in the NHS. This is because there is not enough evidence that this treatment is effective, and it is expensive.
Stoma formation
If other treatments have not worked, you may be offered an operation to remove the rectum. This allows the fistula to heal. The bowel is brought to the surface of the tummy as a stoma. Poo is then collected outside the body in a bag. Find out more in Surgery for Crohn's Disease.
Bowel to bladder fistulas
Less is known about the best treatment for bowel to bladder fistulas. Treatment can include a combination of:
- Medicines such as steroids, infliximab or azathioprine
- Antibiotics. Symptoms like needing to pee suddenly or very often, burning, or passing blood can be signs of a urine infection. You may need to take antibiotics to treat a urine infection.
- Surgery
- Resting the bowel. You may get a liquid food mixture into the bloodstream through a needle in the vein. Having liquid food straight into the blood stream stops food from coming into contact with any inflamed bowel.
Generally, medicines are used first to try and control inflammation. If medicines do not work, your IBD team may talk to you about the option of surgery. Surgery aims to remove the affected bowel, join up the healthy bowel and close the hole in bladder wall. This may be carried out in stages. As well as your IBD team, a specialist from the urology department may also be involved in your care.
Vaginal fistulas
Like bowel to bladder fistulas, less is known about vaginal fistulas. Treatment involves a combination of medicine and surgery. Immunosuppressants, infliximab and antibiotics may help treat the underlying inflammation.
Operations for vaginal fistulas include:
- Draining any abscesses with a seton
- Folding a flap of healthy tissue over the fistula opening (vaginal advancement flap)
- Using the fat pad inside the outer vaginal lip to close the fistula (modified Martius graft)
These operations can be difficult, so specialist surgeons will usually perform them. You are likely to have a team of different surgeons. These could include people specialised in urology, gynaecology and colorectal surgery.
Bowel to skin fistulas
For some bowel to skin fistulas, the fistula may close on its own. But if the fistula stays open for longer than two months this is not likely. If only a small amount of gut contents leaks out of the fistula then medicines like infliximab can be used. If lots of gut contents are leaking out it is more likely surgery is needed. Surgery for bowel to skin fistulas can be difficult. It is affected by factors such as the position of the fistula and how active your Crohn's or Colitis is. Your surgeon will remove the affected bowel, join up the healthy bowel, and then closes the fistula opening on the tummy. People with bowel to skin fistulas may need to stay in hospital for long periods of time.
For bowel to skin fistulas, your body’s fluid and salt levels are monitored and replaced if needed. Tell your IBD team or GP if the amount your fistula leaks changes from what is normal for you. They might need to assess your fluid and salt levels. A drainage bag can be positioned over the area where the fistula opens to collect any leakage. Your skin will need to be protected from the irritant effects of the gut contents, as these can injure the skin.
Some people with bowel to skin fistulas do not absorb enough nutrients from their food. They may also lose nutrients through the opening in the skin. This can be treated by a special liquid only diet. Find out more in Food.
Bowel to bowel fistulas
Bowel to bowel fistulas do not often need any treatment and they may heal by themselves. But surgery may be needed if there is an abscess or narrowing of the bowel. Here, the unhealthy bowel is removed and the fistula opening in the healthy bowel is stitched. Like bowel to skin fistulas, people with bowel-to-bowel fistulas may be low in nutrients. This can be treated by a special liquid only diet. Find out more in Food.